- Acne
- Actinic Keratosis
- Aesthetics
- Alopecia
- Atopic Dermatitis
- Buy-and-Bill
- COVID-19
- Case-Based Roundtable
- Chronic Hand Eczema
- Chronic Spontaneous Urticaria
- Drug Watch
- Eczema
- General Dermatology
- Hidradenitis Suppurativa
- Melasma
- NP and PA
- Pediatric Dermatology
- Pigmentary Disorders
- Practice Management
- Precision Medicine and Biologics
- Prurigo Nodularis
- Psoriasis
- Psoriatic Arthritis
- Rare Disease
- Rosacea
- Skin Cancer
- Vitiligo
- Wound Care
Publication
Article
Dermatology Times
COVID-19 study shows impact on patients with PsO, other autoimmune problems
Author(s):
Ardon Health patients with autoimmune conditions have expressed common questions and concerns about COVID-19.
Recent studies have analyzed how individuals with autoimmune conditions prescribed specialty medications may be affected by the coronavirus disease 2019 (COVID-19) pandemic. Results of several studies were presented during a session of the National Association of Specialty Pharmacy 2020 Annual Meeting & Expo Virtual Experience, along with provider resources for guidelines in managing these chronic conditions and medications with the virus.1
During the session “State of Care: Autoimmune Disorders,” presenter Kate Jelline, PharmD, CSP, MSCS, director of pharmacy operations at Ardon Health, said her health care system has had experiences in helping patients with autoimmune disorders manage their chronic conditions and medications during the COVID-19 pandemic. According to Jelline, Ardon Health patients with autoimmune conditions have expressed common questions and concerns about COVID-19.
“Patients were concerned that the package they receive their medication in was going to have the coronavirus on it from transportation. We also saw these questions very closely aligned with the media. So when the media started showing news stories about supply chain issues, we started getting calls about that,” Jelline said.
Common questions included the following:
- Am I at extra risk for COVID-19 because I am taking an immune-suppressing medication?
- Are there going to be supply issues with getting my medication?
- What extra steps should I take to protect myself?
- Should I stop taking my medication?
- If the medication I am taking is being used in COVID-19 studies, does this mean I am protected?
Jelline said patients became interested in potential COVID-19 benefits through their current medications when the news reported that some of these drugs were being studied for possible treatment of the virus. Although all the answers are not yet known, Jelline said, she shared data from nonrandomized trials relevant to patients with autoimmune conditions.
NYU Langone Health Case Series1,2
In presenting the data, Jelline noted that New York is “an area that was hit very hard by the pandemic early on.” This study analyzed 86 patients with immune-mediated inflammatory disease, of whom 69% had confirmed cases of COVID-19 and 31% were highly expected to have had the virus.
Overall, 72% of the 86 patients were receiving biologics or JAK inhibitors. The study results showed a hospitalization rate of approximately 11%, which the authors concluded was similar to the rate of hospitalization in the general population in New York, according to Jelline.
However, the overall incidence of hospitalization for all 86 patients was 16%. According to Jelline, the results published in the New England Journal of Medicine showed the rate of hospitalization rose above that of the general population for those patients with immune-mediated inflammatory disease who were using oral glucocorticoids, hydroxychloroquine, or methotrexate.
Global Rheumatology Alliance Registry Case Series1,3
This study examined 600 cases of COVID-19 in patients with rheumatic disease, 46% of whom were hospitalized for treatment of the virus. Nine percent of the 600 patients died. Jelline said the study revealed some interesting data.
“The authors looked at the impact of various medications and found that prednisone doses greater than or equal to 10 mg/day were associated with higher risks of hospitalization,” Jelline said.
Conversely, the use of tumor necrosis factor α inhibitors (TNFi) was associated with a reduced risk of hospitalization (odds ratio [OR], 0.40; 95% CI, 0.19-0.81). However, investigators found that conventional synthetic disease-modifying antirheumatic drugs alone or in combination with biologics or JAK inhibitors were not associated with a higher risk of hospitalization (OR, 1.23; 95% CI, 0.70- 2.17; and OR, 0.74; 95% CI, 0.37-1.46), respectively.
Lombardy, Italy, Case Control1,4
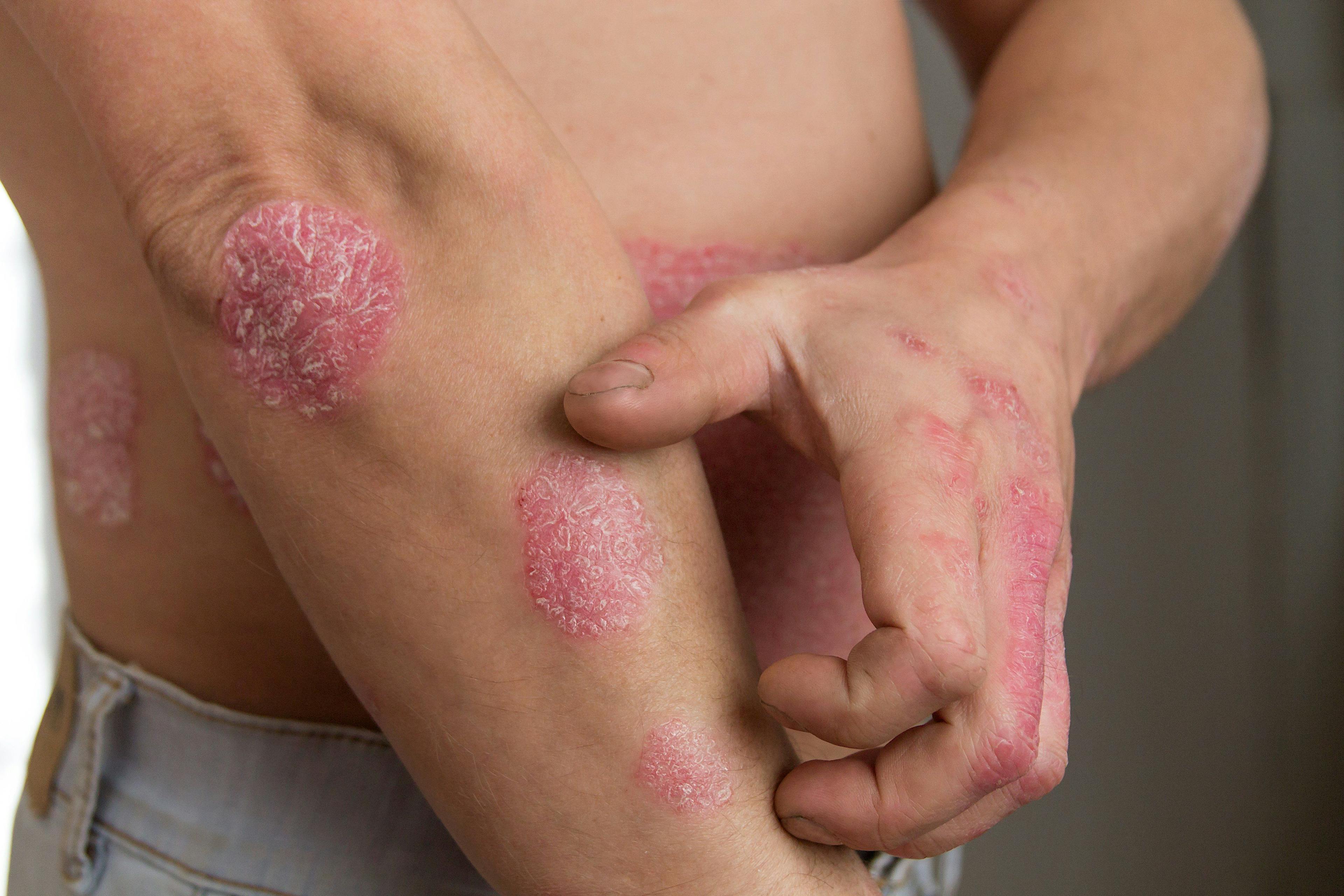
This study found that patients with psoriasis (PsO) who were being treated with biologics had a higher risk of testing positive for COVID-19 (OR, 3.43; 95% CI, 2.25-5.73), needing to self-quarantine at home (OR, 9.05; 95% CI, 5.61-14.61), and needing hospitalization (OR, 3.59; 95% CI, 1.49-8.63) compared with the general population.
“However, there was no increased risk of [intensive care unit] admission or death,” Jelline said.
This controlled study examined 1193 patients with plaque PsO, most of whom were treated with biologics. They included patients treated with IL-17 inhibitors (45.0%), TNFi (22.0%), IL-12/23 inhibitors (20.0%), PDE4 inhibitors (6.5%), and IL-23 inhibitors (5.0%).1
“[This is] another area hit particularly hard by the pandemic,” Jelline said.
According to the investigators, only 17 patients with PsO and confirmed cases of COVID-19 were quarantined at home, and 5 were hospitalized; no patients with PsO and COVID-19 were admitted to the intensive care unit or died.4 Investigators recommended that patients with PsO who are taking biologics be monitored at home through telemedicine during the pandemic.4
Conclusions
Jelline said a better understanding of COVID-19 and its potential risks to patients with autoimmune conditions on specialty medications will, hopefully, come as more is learned about the virus and more robust trial data become available.
Until then, pharmacists can use COVID-19 guidelines to manage autoimmune conditions in patients. Jelline briefly touched on some familiar organizations that offer guidance to pharmacists. The American College of Rheumatology, for example, provides recommendations about what to do in certain scenarios, such as when and how long to hold biologics and JAK inhibitors in cases of virus exposure.
“This guidance continues to be updated very frequently due to rapidly expanding information and evolving evidence as we learn more about the virus,” Jelline said.
Other sources for provider guidance include the American Academy of Dermatology, the Multiple Sclerosis International Federation, the American Gastroenterological Association, the Arthritis Foundation, the Crohn’s & Colitis Foundation, the Lupus Foundation of America, the National Multiple Sclerosis Society, the National Psoriasis Foundation, and the Spondylitis Association of America.
This article was originally posted by our sister publication Pharmacy Times.
References:
- Jelline K, Riccardo C. State of care 2020: autoimmune disorders. Presented at: National Association of Specialty Pharmacy 2020 Annual Meeting & Expo Virtual Experience; September 17, 2020.
- Haberman R, Axelrad J, Chen A, et al. COVID-19 in immune-mediated inflammatory diseases—case series from New York. N Engl J Med. 2020;383(1):85-88. doi:10.1056/NEJMc209567
- Gianfrancesco M, Hyrich KL, Al-Adely S, et al. Characteristics associated with hospitalisation for COVID-19 in people with rheumatic disease: data from the COVID-19 Global Rheumatology Alliance physician-reported registry. Ann Rheum. Dis. 2020;79(7):859-866. doi:10.1136/annrheumdis-2020-217871
- Damiani G, Pacifico A, Bragazzi NL, Malagoli P. Biologics increase the risk of SARS-CoV-2 infection and hospitalization, but not ICU admission and death: real-life data from a large cohort during red-zone declaration. Dermatol Ther. Published online May 1, 2020. doi:10.1111/dth.13475

Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.